Trauma-Informed Care (TIC)
Examples of trauma include, but are not limited to:
- Experiencing or observing physical, sexual and emotional abuse.
- Being neglected in childhood.
- Having a family member with a mental health or substance use disorder.
- Experiencing or witnessing violence in the home, community, or while serving in the military.
- Experiencing poverty and system discrimination.
Widespread adoption of trauma-informed care is essential given the prevalence and impact of trauma within the homeless population.
Hopper et al define Trauma-Informed Care (TIC) as “a strengths-based framework that is grounded in an understanding of and responsiveness to the impact of trauma, that emphasizes physical, psychological, and emotional safety for both clinicians and survivors, and that creates opportunities for survivors to rebuild a sense of control and empowerment.”45
TIC is more than a treatment method or idea. TIC aims to recognize human behavior, positive and negative coping strategies, and other issues that result from the experience of trauma over the lifespan.46 TIC promotes a culture of safety, empowerment and healing not only for patients but for organizations and staff. It may require organizational culture change.
The following are the basic principles of Trauma-informed care47:
- Safety: Making sure patients feel physically and emotionally safe in their health care setting.
- Patient Empowerment: Allowing patients to take an active role in their treatment using a strengths-based approach.
- Voice and Choice: Using shared decision-making.
- Collaboration and Mutuality: Including staff, patients, and their families or social workers in clinical and organizational planning.
- Trustworthiness: Giving clear information about treatment plans and how the care will be provided.
- Cultural, Historic and Gender Issues: Being sensitive to cultural, racial, ethnic, sexual and gender stereotypes and biases, offering the preferred cultural treatments, and acknowledging the existence of multigenerational trauma.
a) Re-traumatization.
The term re-traumatization describes a conscious or unconscious reminder of past trauma that results in a re-experiencing of the initial trauma event. It can be triggered by a clinical practice, setting, or staff attitudes and can occur with patients and staff.
Given the prevalence of trauma survivors within the homeless population, communication and treatment should aim to avoid re-traumatization. Be aware of how medical care can re-traumatize during48:
- Invasive procedures.
- Removal of clothing.
- Physical touch.
- Vulnerable physical position such as a pelvic exam.
- Loss of and lack of privacy.
- Time-limited, pressured or rushed encounters.
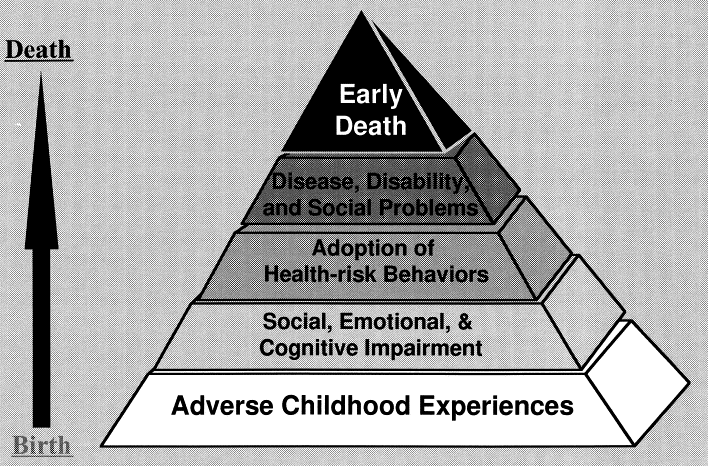
b) Adverse Childhood Experiences (ACE)
The CDC defines Adverse Childhood Experiences (ACEs) as “potentially traumatic events that occur in childhood (0-17 years), such as experiencing violence, abuse, or neglect; witnessing violence in the home or community; or having a family member attempt or die by suicide. Also included are aspects of the child’s environment that can undermine their sense of safety, stability, and bonding such as growing up in a household with substance misuse, mental health problems, or instability due to parental separation or incarceration of a parent, sibling, or other member of the household.” ACEs are related to chronic health problems, mental illness and substance misuse in adults and can have detrimental effects on education and job opportunities.49
Guarino et al’s Key Implications for Homeless Populations with Backgrounds of Trauma are as follows52:
- “Integrating Care—Maintaining a holistic view of consumers and their process of healing and facilitating communication within and among service clinicians and systems.
- Healing Happens in Relationships—Believing that establishing safe, authentic and positive relationships can be corrective and restorative to survivors of trauma.
- Recovery is Possible—Understanding that recovery is possible for everyone regardless of how vulnerable they may appear; instilling hope by providing opportunities for consumer and former consumer involvement at all levels of the system, facilitating peer support, focusing on strength and resiliency, and establishing future-oriented goals.”